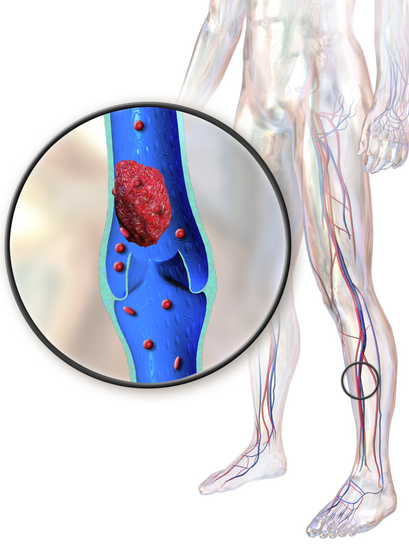
Deep vein thrombosis (DVT) is caused by a blood clot in a deep vein. Usually this happens in the lower extremities of the body, such as in the calves. Often when DVT occurs it is because of a few factors that include immobility (travel), surgery (knee or hip replacement), hormone therapy, pregnancy, and medical conditions. In essence these factors result in blood pooling in the lower extremities (usually the calves), which then makes it more likely for DVT to occur.
Symptoms
A lot of the time DVT causes no symptoms, because of this it is important to note that being over 60 years of age, smoking, being overweight, surgery, or sitting for long periods of time are all risk factors for DVT. Precautionary measures should be taken when these risk factors are present.
If symptoms do appear there will be:
- Swelling in one or both legs
- Pain/Tenderness in one or both legs, even when just standing or walking
- Skin on legs are warm
- Red or discolored skin on the legs
- Veins you can see that are swollen, red, hard or tender when touched
Pulmonary Embolism
If these symptoms are present it is important to go to an emergency room (ER) to properly be evaluated and diagnosed. The reason for going to the ER, is because a life threatening condition called pulmonary embolism (PE) could develop. Possible symptoms for PE are:
- Suddenly coughing up blood
- Sharp chest pain or tightness in the chest
- Pain in the shoulder, arm, back, or jaw
- Rapid breathing and/or shortness of breath
- Pain when breathing
- Fast heart beat
- Sever lightheadedness
Pulmonary embolism is a condition caused by a blood clot that breaks free from clotted blood in the legs. This blood clot can travel through the blood stream to the lungs, heart or brain which can cause death. About 1 in 10 people who have DVT will have PE and it is possible that number could be higher since PE often has no symptoms and goes undiagnosed.
It should be noted that the combination of having Deep Vein Thrombosis and a Pulmonary Embolism is sometime referred to Venous Thromboembolism.
Treatment for Deep Vein Thrombosis
There are a number of ways to treat DVT, such as with blood thinner medication, surgery, vena cava filter, or venous thrombectomy. In most cases blood thinner medication is the best and most effective treatment.
Preventing Deep Vein Thrombosis
If there is a high risk of getting DVT (because of immobility, surgery, hormone therapy, pregnancy, and medical conditions) the use of an intermittent pneumatic compression (IPC) device can be used to decrease the chances of DVT. IPC are devices that have cuffs that wrap around the leg that fill with air to squeeze the leg. This squeezing increases blood flow through the vein which helps to prevent blood clots.
IPC treatment is most often done in hospitals, but can be done at home. There are different kinds of IPC devices. Some wrap around the calf only and some may wrap around the entire leg. Some device may inflate around the lower part of the leg (calf) and then inflate around the upper part of leg (quads). Some devices may inflate around the whole leg all at once. Some device inflate slow and some fast.
The device will cycle through inflating and deflating repeatedly, hence why the word intermittent is used to describe the treatment.
Because DVT is often caused by blood pooling in lower extremities to prevent DVT that pooled blood needs to be moved through the veins. This is done by the squeezing action of IPC devices which pushes blood through the veins. Then when that squeezing action is released blood flows back into the veins. Basically, IPC's act like a pump pushing blood through the veins back towards the heart.
Risks of Intermittent Pneumatic Compression
Just like any treatment, there are risks. The risks include:
- Skin breakdown (most likely to happen individuals older than 60)
- Discomfort, warmth, and/or sweating beneath the cuff
- Pressure injury (not likely to happen)
- Nerve damage (not likely to happen)
When you remove the device to shower, make sure to check the skin for tenderness, swelling, warmth, redness, or skin breakdown. If this is happening let your healthcare provider know. Make sure to put it back on as soon as possible. The more the IPC is used, the less likely DVT and PE will occur.